10/22/2020 What The New CDC Definition Of A COVID-19 'Close Contact' Means For You, by Lindsay Holmes, Huffpost
The updated guidance now defines close contact as being within 6 feet of someone with the virus for a cumulative total of 15 minutes (or more) over a 24-hour period.
The CDC previously defined close contact as being within 6 feet of someone infected with COVID-19 for at least 15 minutes or more.
The pool of individuals considered close contacts will get a lot bigger with this new guidance ― especially when you consider interactions in schools and businesses, Caitlin Rivers, an epidemiologist at the Johns Hopkins Center for Health Security, told The Washington Post.
“It’s easy to accumulate 15 minutes in small increments when you spend all day together — a few minutes at the water cooler, a few minutes in the elevator, and so on,” Rivers said. “I expect this will result in many more people being identified as close contacts.”
10/22/2020 Stop wiping down groceries and focus on bigger risks, say experts on coronavirus transmission, by Elizabeth Chang, The Washington Post
Protection is not gained by washing down everything in the environment, Morens said. “It’s the behaviors you do to make sure that nothing in the environment, including your own hands, gets into your mouth, nose or eyes.”
Those behaviors include never touching yourself above the neck, wearing a mask (which also helps remind you not to touch your face), social distancing and making sure your hands are as clean as possible. In that case, you could even go into a restaurant and touch objects there — the chair, the menu — without wiping them down first, and “if the very last thing you touch is soap and water or hand sanitizer … you’re okay,” said Morens.
?
6/16/2020: Put a lid on it, folks: Flushing may release coronavirus-containing ‘toilet plumes’, by Karin Brulliard and William Wan, The Washington Post
For all our paranoia about the surface of toilet seats — the tissue paper we oh-so-carefully lay down, the thin covers often offered in public stalls — germ transmission from skin contact is a relatively small health risk compared with what happens after you flush. That’s when bits of fecal matter swish around so violently that they can be propelled into the air, become aerosolized and then settle on the surroundings.
Experts call it the “toilet plume.”
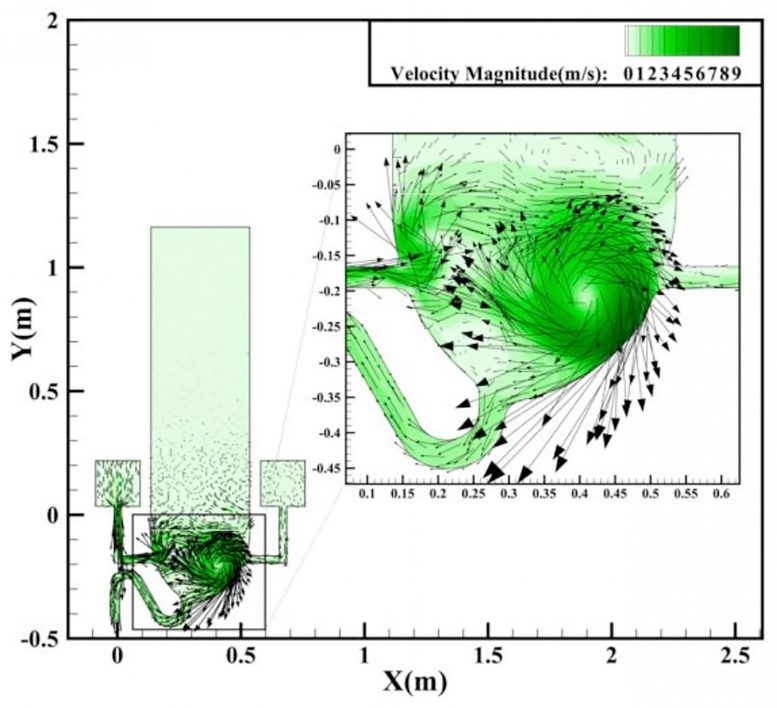
The simulations show that nearly 60% of the ejected particles rise high above the seat for a toilet with two inlet ports. A solution to this deadly problem is to simply close the lid before flushing, since this should decrease aerosol spread.
However, in many countries, including the United States, toilets in public restrooms are often without lids. This poses a serious hazard. The investigators also suggest a better toilet design would include a lid that closes automatically before flushing.
6/16/2020: Can a toilet promote virus transmission? From a fluid dynamics perspective, by Yun-yun Li, Ji-Xiang Wang and Xi Chen, Physics of Fluids
The volume-of-fluid (VOF) model is used to simulate two common flushing processes (single-inlet flushing and annular flushing), and the VOF–discrete phase model (DPM) method is used to model the trajectories of aerosol particles during flushing. The simulation results are alarming in that massive upward transport of virus particles is observed, with 40%–60% of particles reaching above the toilet seat, leading to large-scale virus spread.
Video: How a serious nation protects its children
5/28/2020: To Beat Covid-19, You Have to Know How A Virus Moves, by Adam Rogers, Wired
TO REALLY UNDERSTAND how the disease Covid-19 spreads, you have to see the world the way a virus moves through it. It’s just a fleck of protein and genes, a little bit of code in a package with no to-do list beyond hijacking the biology of living things to make copies of itself and spread them to other living things. What happens to those other living things in the process—maybe they get sick, maybe they die—isn’t the virus’s problem. Viruses don’t have problems.
The virus lives in the deep lungs, and it has to get up and out of the nose and throat for transmission. Some researchers looking into the Washington choir cluster suggested that the deep breaths and powerful exhalations required for singing carried more virus, making that outbreak worse (even though it turned out that the singers had in fact gotten inside each other’s social-distance force fields). Ristenpart’s team at UC Davis has found that simple talking gives off 1 to 50 particles per second, with louder talking corresponding to higher numbers. That might be due to something called the “fluid-film burst mechanism”; when you inhale, the air-gathering sacs of the lungs, the alveoli, expand and stretch the thick fluid that lines them. It pops and splashes a bit, pinching off the tiny aerosol particles. And that part of the lungs is exactly where the virus is more likely to live. “The physicists have accepted this,” says Robin Wood, director of the Desmond Tutu HIV Foundation in Cape Town, South Africa, and an expert in the airborne transmission of tuberculosis, “whereas the physicians haven’t really got to understand it.”
5/27/2020: Reducing transmission of SARS-CoV-2, Kimberly A. Prather, Chia C. Wang, Robert T. Schooley, Science
The World Health Organization (WHO) recommendations for social distancing of 6 ft and hand washing to reduce the spread of SARS-CoV-2 are based on studies of respiratory droplets carried out in the 1930s. These studies showed that large, ~100 μm droplets produced in coughs and sneezes quickly underwent gravitational settling (1). However, when these studies were conducted, the technology did not exist for detecting submicron aerosols.
As a comparison, calculations predict that in still air, a 100-μm droplet will settle to the ground from 8 ft in 4.6 s whereas a 1-μm aerosol particle will take 12.4 hours (4). Measurements now show that intense coughs and sneezes that propel larger droplets more than 20 ft can also create thousands of aerosols that can travel even further (1). Increasing evidence for SARS-CoV-2 suggests the 6 ft WHO recommendation is likely not enough under many indoor conditions where aerosols can remain airborne for hours, accumulate over time, and follow air flows over distances further than 6 ft (5, 10).
Traditional respiratory disease control measures are designed to reduce transmission by droplets produced in the sneezes and coughs of infected individuals. However, a large proportion of the spread of coronavirus disease 2019 (COVID-19) appears to be occurring through airborne transmission of aerosols produced by asymptomatic individuals during breathing and speaking (1–3). Aerosols can accumulate, remain infectious in indoor air for hours, and be easily inhaled deep into the lungs. For society to resume, measures designed to reduce aerosol transmission must be implemented, including universal masking and regular, widespread testing to identify and isolate infected asymptomatic individuals
5/21/2020: Virus ‘does not spread easily’ from contaminated surfaces or animals, revised CDC website states, by Ben Guarino and Joel Achenbach, Washington Post
5/19/2020: Yikes! Saliva Droplets From Mild Cough Travel Up to 18 Feet, Talib Dbouk and Dimitris Drikakis, Physics of Fluids, (SciTechDaily)
5/19/2020: On coughing and airborne droplet transmission to humans, by Talib Dbouk and Dimitris Drikakis, Physics of Fluids
5/14/2020: New York Times: Talking Can Generate Coronavirus Droplets That Linger Up to 14 Minutes, by Knvul Sheikh
Coughs or sneezes may not be the only way people transmit infectious pathogens like the novel coronavirus to one another. Talking can also launch thousands of droplets so small they can remain suspended in the air for eight to 14 minutes, according to a new study.
5/13/2020: PNAS: The airborne lifetime of small speech droplets and their potential importance in SARS-CoV-2 transmission, by Valentyn Stadnytskyi, Christina E. Bax, Adriaan Bax and Philip Anfinrud
Highly sensitive laser light scattering observations have revealed that loud speech can emit thousands of oral fluid droplets per second. In a closed, stagnant air environment, they disappear from the window of view with time constants in the range of 8 to 14 min, which corresponds to droplet nuclei of ca. 4 μm diameter, or 12- to 21-μm droplets prior to dehydration. These observations confirm that there is a substantial probability that normal speaking causes airborne virus transmission in confined environments.
5/17/2020: NIH Begins Clinical Trial of Hydroxychloroquine and Azithromycin to Treat COVID-19, NIH, (SciTechDaily)
5/15/2020: Drug promoted by Trump as coronavirus ‘game changer’ increasingly linked to deaths, by Toluse Olorunnipa, Ariana Eunjung Ch and Laurie McGinley, Washington Post
4/20/2020: Can You Spread the Virus Just by Speaking?, by David Axe, Daily Beast
The virus that causes COVID-19 could be a lot easier to spread than many people realize. It might even be possible to give somebody the SARS-CoV-2 virus by simply talking to them, a team of scientists concluded.
New England Journal of Medicine: Visualizing Speech-Generated Oral Fluid Droplets with Laser Light Scattering, by Philip Anfinrud, Valentyn Stadnyskyi (NIH) and Christina E. Bax (Penn)
The act of speaking generates oral fluid droplets that vary widely in size,1 and these droplets can harbor infectious virus particles. Whereas large droplets fall quickly to the ground, small droplets can dehydrate and linger as “droplet nuclei” in the air, where they behave like an aerosol and thereby expand the spatial extent of emitted infectious particles.2 We report the results of a laser light-scattering experiment in which speech-generated droplets and their trajectories were visualized.
Advances in Virology: The Effects of Temperature and Relative Humidity on the Viability of the SARS Coronavirus, by K.H. Chan, et al, Oct 1, 2011
Caveat: This communication describes effects on a related coronavirus.
Wired: How to Clean and Disinfect Yourself, Your Home, and Your Stuff, by Jess Grey, 4/9/2020
WHO: Rumours and Facts on COVID-19, Issue #2
Los Angeles Times: How to keep your coronavirus face mask clean, by Andrea Castillo, 4/4/2020
CNN: Experts tell White House coronavirus can spread through talking or even just breathing, By Elizabeth Cohen,4/2/2020
Cleveland.com: Michigan recommends everyone ‘strongly consider’ wearing masks in public to stop coronavirus. by Laura Johnstone, 4/2/2020
Michigan Chief Medical Executive Dr. Joneigh Khaldun said residents should “strongly consider” wearing homemade masks in public to protect themselves and their community from the coronavirus.
The Atlantic: Everyone Thinks They’re Right About Masks, by Ed Yong, 4/4/2020 update
If the Nebraska team does find infectious particles, it would mean that even mildly symptomatic people can expel SARS-CoV-2 into the air, and that the virus can travel at least the length of a hospital room—a claim supported by a few other studies. Even that, though, would not guarantee danger. Are those far-spreading virus particles concentrated enough to infect another person in the same room? How many virus particles does it even take to launch an infection? How far does the virus travel in outdoor spaces, or in other indoor settings? Have these airborne movements affected the course of the pandemic?
Wired: It's Time to Face Facts, America: Masks Work, by Ferris Jabr, 3/28/2020
WHEN YOU LOOK at photos of Americans during the 1918 influenza pandemic, one feature stands out above all else: masks. Fabric, usually white gauze, covers nearly every face.
MLive: Michigan doctor says leave groceries outside for 3 days if possible, shows how to disinfect, by Justine Lofton, 3/28/2020
Jeffrey VanWingen, MD, a doctor at Family Medicine Specialists, created a 13-minute video to show everyone how to bring food into their homes as safely as possible.
“Imagine that your groceries are covered in glitter, and your goal at the end of this is to not have any glitter in your house, on your hands or, especially, on your face,” VanWingen said. “Imagine that disinfectants and soap have the power to dissolve that glitter.”
“This all seems a bit time consuming, but, in truth, these days people do have a bit more time on their hands," VanWingen said. “Let’s be methodical and be safe, and not take any chances.”
Youtube video: Safe Grocery Shopping in COVID-19 Pandemic, Jeffrey VanWingen MD
MLive: 11 ways to make grocery shopping safer as coronavirus spreads, by Justine Lofton, 3/26/2020
The New York Times: More Americans Should Probably Wear Masks for Protection, Knvul Sheikh, 3/27/2020
When researchers conducted systematic review of a variety of interventions used during the SARS outbreak in 2003, they found that washing hands more than 10 times daily was 55 percent effective in stopping virus transmission, while wearing a mask was actually more effective — at about 68 percent. Wearing gloves offered about the same amount of protection as frequent hand-washing, and combining all measures — hand-washing, masks, gloves and a protective gown — increased the intervention effectiveness to 91 percent.
National Geographic: How some cities ‘flattened the curve’ during the 1918 flu pandemic, by Nina Strochlic and Riley D. Champine, 3/27/2020
The 1918 flu, also known as the Spanish Flu, lasted until 1920 and is considered the deadliest pandemic in modern history. Today, as the world grinds to a halt in response to the coronavirus, scientists and historians are studying the 1918 outbreak for clues to the most effective way to stop a global pandemic. The efforts implemented then to stem the flu’s spread in cities across America—and the outcomes—may offer lessons for battling today’s crisis. (Get the latest facts and information about COVID-19.)
US National Library of Medicine / BMJ: Physical interventions to interrupt or reduce the spread of respiratory viruses: systematic review, by Jefferson, Foxlee, Del Mar, Dooley, Ferroni, Hewak, Prabhala, Nair, Rivetti, 1/12/2008
Meta-analysis of six case-control studies suggests that physical measures are highly effective in preventing the spread of SARS: handwashing more than 10 times daily (odds ratio 0.45, 95% confidence interval 0.36 to 0.57; number needed to treat=4, 95% confidence interval 3.65 to 5.52); wearing masks (0.32, 0.25 to 0.40; NNT=6, 4.54 to 8.03); wearing N95 masks (0.09, 0.03 to 0.30; NNT=3, 2.37 to 4.06); wearing gloves (0.43, 0.29 to 0.65; NNT=5, 4.15 to 15.41); wearing gowns (0.23, 0.14 to 0.37; NNT=5, 3.37 to 7.12); and handwashing, masks, gloves, and gowns combined (0.09, 0.02 to 0.35; NNT=3, 2.66 to 4.97).
Michigan Public Radio: WHO Reviews 'Current' Evidence On Coronavirus Transmission Through Air, Nell Greenfieldboyce, 3/28/2020
The World Health Organization says the virus that causes COVID-19 doesn't seem to linger in the air or be capable of spreading through the air over distances of more than about 3 feet. But at least one expert in virus transmission said it's way too soon to know that.
"I think the WHO is being irresponsible in giving out that information. This misinformation is dangerous," says Dr. Donald Milton, an infectious disease aerobiologist at the University of Maryland's School of Public Health.
"I don't think they know, and I think they are talking out of their hats," Milton says.
UCLA: How Long COVID-19 Remains Infectious on Cardboard, Metal & Plastic, UNIVERSITY OF CALIFORNIA - LOS ANGELES, 3/27/2020
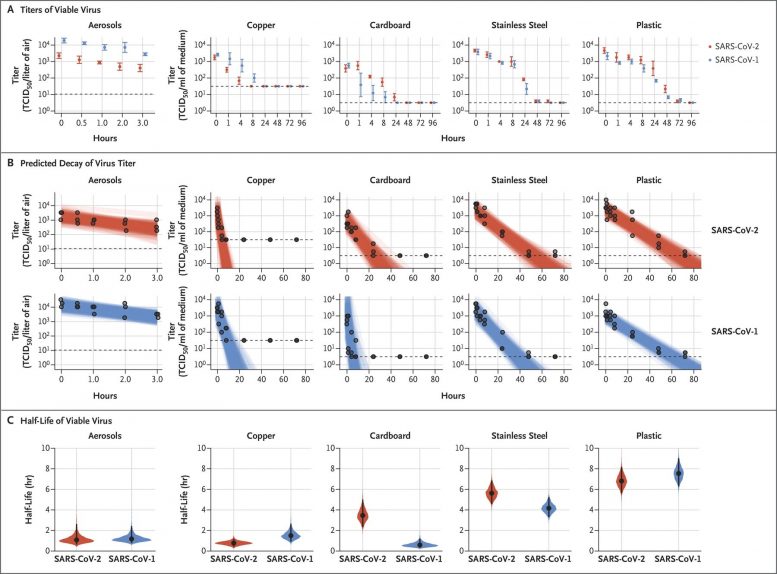
Viability of SARS-CoV-1 and SARS-CoV-2 in Aerosols and on Various Surfaces. Credit: NEJM
NPR: Experts on leaving the house: if you touch stuff, wash your hands, 3/27/2020
Associate Professor of Medicine at Michigan State University Peter Gulick advises carrying a spray bottle of disinfectant. He says using wipes alone just smears things around and he prefers spraying the key pad and then wiping before you use it.
Gulick says rather than picking individual fruit such as oranges or apples, buy a bag. At least the fruit is not directly handled by other people. Then wash your fruit like you should be doing anyway.
Ask a person handing you takeout food to put it in the seat or pop the trunk and have them put it there.
Washington Post: The coronavirus isn’t alive. That’s why it’s so hard to kill, by Sarah Kaplan, William Wan, and Joel Achenblach, 3/23/2020
Viruses have spent billions of years perfecting the art of surviving without living — a frighteningly effective strategy that makes them a potent threat in today’s world.
That’s especially true of the deadly new coronavirus that has brought global society to a screeching halt. It’s little more than a packet of genetic material surrounded by a spiky protein shell one-thousandth the width of an eyelash, and it leads such a zombielike existence that it’s barely considered a living organism.
Washington Post: What the structure of the coronavirus can tell us, by Bonnie Berkowitz, Aaron Steckelberg and John Muyskens, 3/23/2020
After about 20 seconds of contact, soap breaks apart the fragile, fatty membrane that holds the virus together. Disinfecting agents with at least 60 percent alcohol puncture and destroy the virus in a similar way.
Extreme heat — near boiling — causes the proteins in the spikes to unravel and lose their shape, deactivating them. (A human fever is not hot enough to do this; it’s unclear what effect warm summer weather will have.)
Ultraviolet light has been used as a disinfectant for a century in hospitals and water supplies. It shatters the genetic material inside viruses, bacteria and other microbes. However, it doesn’t always work uniformly, Menachery said, and disinfecting UV light can’t be used with people around because it damages human cells.

Boston Career Institute: Lecture on Disinfection
The principle and importance of wetting surfaces for the Labeled amount of time is demonstrated in the above video
EPA: List N Disinfectants for use against SARS-COV-2, the Coronavirus that causes the disease COVID-19
LensRentals: How to Disinfect Camera Equipment and Spaces, Roger Cicala, 3/20/2020
Science Daily: Singapore modelling study estimates impact of physical distancing on reducing spread of COVID-19, 3/24/2020
- Source: The Lancet
Science Daily: Study reveals how long COVID-19 remains infectious on cardboard, metal and plastic, 3/20/2020
- The study: Journal of the American Medical Association,
- The study's authors are from UCLA, the National Institutes of Health's National Institute of Allergy and Infectious Diseases, the Centers for Disease Control and Prevention, and Princeton University.
Reference: “Aerosol and Surface Stability of SARS-CoV-2 as Compared with SARS-CoV-1” 17 March 2020, New England Journal of Medicine.
DOI: 10.1056/NEJMc2004973Authors:
Neeltje van Doremalen, Ph.D.
Trenton Bushmaker, B.Sc.
National Institute of Allergy and Infectious Diseases, Hamilton, MTDylan H. Morris, M.Phil.
Princeton University, Princeton, NJMyndi G. Holbrook, B.Sc.
National Institute of Allergy and Infectious Diseases, Hamilton, MTAmandine Gamble, Ph.D.
University of California, Los Angeles, Los Angeles, CABrandi N. Williamson, M.P.H.
National Institute of Allergy and Infectious Diseases, Hamilton, MTAzaibi Tamin, Ph.D.
Jennifer L. Harcourt, Ph.D.
Natalie J. Thornburg, Ph.D.
Susan I. Gerber, M.D.
Centers for Disease Control and Prevention, Atlanta, GAJames O. Lloyd-Smith, Ph.D.
University of California, Los Angeles, Los Angeles, CA, Bethesda, MDEmmie de Wit, Ph.D.
Vincent J. Munster, Ph.D.
National Institute of Allergy and Infectious Diseases, Hamilton, MTSupported by the Intramural Research Program of the National Institute of Allergy and Infectious Diseases, National Institutes of Health, and by contracts from the Defense Advanced Research Projects Agency (DARPA PREEMPT No. D18AC00031, to Drs. Lloyd-Smith and Gamble), from the National Science Foundation (DEB-1557022, to Dr. Lloyd-Smith), and from the Strategic Environmental Research and Development Program of the Department of Defense (SERDP, RC-2635, to Dr. Lloyd-Smith).
Science Daily: COVID-19 coronavirus epidemic has a natural origin, 3/17/2020
- "By comparing the available genome sequence data for known coronavirus strains, we can firmly determine that SARS-CoV-2 originated through natural processes," said Kristian Andersen, PhD, an associate professor of immunology and microbiology at Scripps Research and corresponding author on the paper.
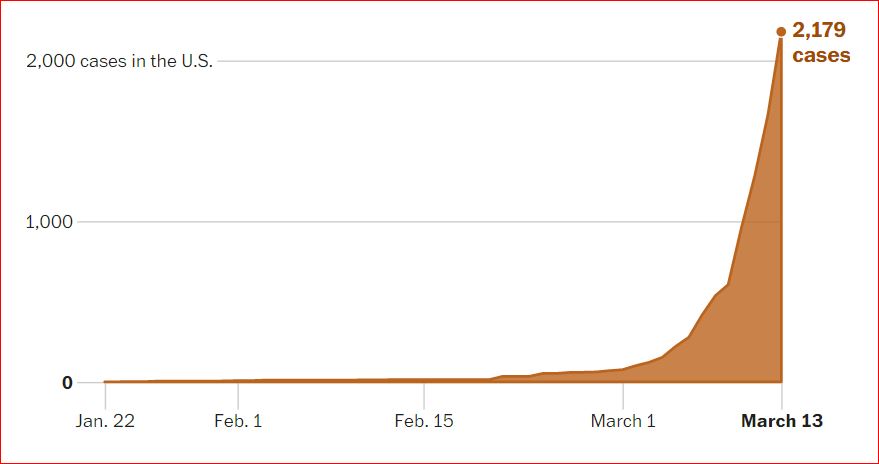
3/14/2020 Why outbreaks like coronavirus spread exponentially, and how to “flatten the curve”, By Harry Stevens, The Washington Post
Wired: They Say Coronavirus Isn't Airborne—but It's Definitely Borne By Air, by Roxanne Khamsi, 3/14/2020
Science Daily: New study on COVID-19 estimates 5.1 days for incubation period, 3/10/2020
- An analysis of publicly available data on infections from the new coronavirus, SARS-CoV-2, that causes the respiratory illness COVID-19 yielded an estimate of 5.1 days for the median disease incubation period, according to a new study led by researchers at Johns Hopkins Bloomberg School of Public Health.
- The analysis suggests that about 97.5 percent of people who develop symptoms of SARS-CoV-2 infection will do so within 11.5 days of exposure. The researchers estimated that for every 10,000 individuals quarantined for 14 days, only about 101 would develop symptoms after being released from quarantine.
Politico: DHS wound down pandemic models before coronavirus struck. 3/24/2020
- The Department of Homeland Security stopped updating its annual models of the havoc that pandemics would wreak on America’s critical infrastructure in 2017, according to current and former DHS officials with direct knowledge of the matter.
- From at least 2005 to 2017, an office inside DHS, in tandem with analysts and supercomputers at several national laboratories, produced detailed analyses of what would happen to everything from transportation systems to hospitals if a pandemic hit the United States.
- But the work abruptly stopped in 2017 amid a bureaucratic dispute over its value, two of the former officials said, leaving the department flat-footed as it seeks to stay ahead of the impacts the COVID-19 outbreak is having on vast swathes of the U.S. economy.
- The models -- primarily computer simulations that seek to anticipate the interaction between millions of Americans and U.S. infrastructure systems -- were overseen by the National Infrastructure Simulation and Analysis Center (NISAC), a program that has been run by a shifting alphabet soup of agencies within DHS, reflecting the continual bureaucratic reshuffling that has plagued the department since its inception in 2002.
- Some of the modeling unit’s analyses looked at what would happen if a large portion of the U.S. workforce — say, 40 percent — got sick or couldn’t show up to work to maintain and operate key aspects of the national infrastructure, such as the systems that keep planes flying safely. The reports were meant to guide policymakers toward areas that would demand their attention in the event of an outbreak.
- One 2015 DHS report, based partly on data produced by NISAC, warned that America’s public and private health systems might “experience significant shortages in vaccines, antivirals, pharmaceuticals needed to treat secondary infections and complications, personal protective equipment (PPE), and medical equipment, including ventilators.”
- Juliette Kayyem, a senior DHS official in the Obama administration, praised the quality of the NISAC reports she received when she was at the department, and criticized DHS for being “singularly focused on border enforcement” under Trump at the expense of properly planning for other threats like a pandemic.
- “We should not be surprised that a department that has for the last three and a half years viewed itself solely as a border enforcement agency seems ill-equipped to address a much greater threat to the homeland,” she said.
- “I’ve heard people say it’s a black swan. It’s not a black swan,” said one of the former DHS officials. “This is the whitest of white swans. This was absolutely inevitable, and the fact is we didn’t even maintain the capacity that we had or even the records of what we had done so that information could be quickly located and turned over to people who are making the critical operations right now.”
Science Daily: 2009 swine flu pandemic originated in Mexico, researchers discover, 6/27/2016
- Source: The Mount Sinai Hospital / Mount Sinai School of Medicine
- Researchers used state-of-the-art genetic analysis to identify the precise location and the main molecular transformations that allowed a pig influenza virus to jump into humans. They found that the virus responsible was a mix of one North American swine virus that had jumped between birds, humans, and pigs, and a second Eurasian swine virus, that circulated for more than 10 years in pigs in Mexico before jumping into humans. Previously, the most closely related ancestor viruses to the 2009 H1N1 virus were identified in Asian swine, but they were not as close genetically to the human 2009 pandemic H1N1 virus as the swine Mexican isolates found in this study.
- The only other H1N1 pandemic flu known to date was the "Spanish" flu of 1918 that killed between 50 and 100 million people -- 3 to 5 percent of the world's population.